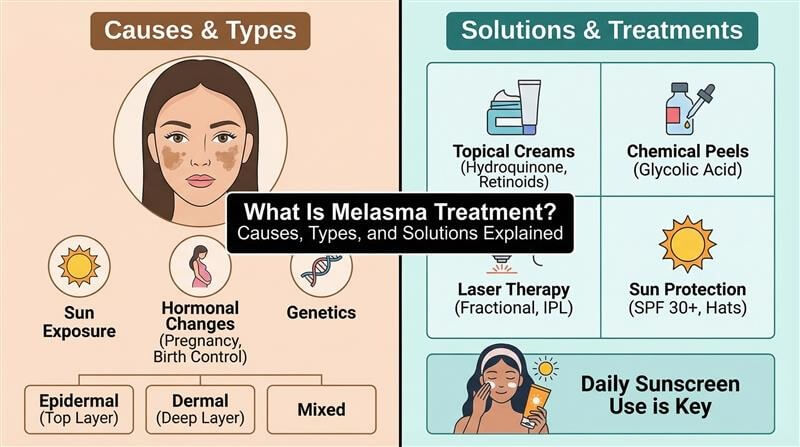
What Is Melasma Treatment? Causes, Types and Solutions Explained
Melasma can feel confusing because it is not “just a dark patch”. It is a long term pigment condition that can fade, flare, and return depending on sun exposure, heat, hormones, and skin irritation from the wrong products. That is why many people search What Is Melasma Treatment when they are tired of trying random creams and want a clear plan that matches their skin.
At TLC Skyn, patients usually ask two practical questions:
- Why did these patches start now?
- What is the safest way to treat melasma without making it worse?
This guide explains what melasma treatment really means, the causes and main types, and the solutions dermatologists commonly use. You will also see trend insights, simple comparisons, and investor style examples that show how people spend wisely (or waste money) when building a treatment plan.
What is melasma treatment?
Melasma treatment is a planned, step by step approach to lighten visible patches and reduce how often they come back. For most people, it is not a one time fix. It is closer to “control” than “cure”, because triggers can reactivate pigment production.
In simple words, melasma treatment usually includes:
- Daily sun and visible light protection
- Topical products
- In clinic options when needed
- Lifestyle and trigger control
A key point: melasma is not the same as a single sunspot. If you treat it like a sunspot, for example with harsh home peeling or aggressive heat based procedures, it can get darker. That is because irritation and inflammation can trigger more pigment.
Why melasma happens
Melasma happens when pigment cells (melanocytes) become overactive and produce too much melanin in certain areas, most often the cheeks, forehead, upper lip, and jawline.
The most common triggers are:
Sun exposure and visible light
UV rays trigger pigment. Visible light can also worsen melasma, especially in deeper skin tones, which is why some people flare even when they “never burn”. The American Academy of Dermatology lists sun protection as a core part of controlling melasma and preventing recurrence.
Hormones
Pregnancy, oral contraceptives, thyroid problems, and other hormonal shifts can trigger or worsen melasma. This is why melasma is more common in women, but men can get it too.
Heat (often underestimated)
Heat can fuel inflammation pathways in the skin and can worsen melasma even without direct sun exposure. For many patients in warm climates, heat management becomes part of the plan.
Skin irritation
Over exfoliation, harsh scrubs, steroid misuse, fragrance heavy products, and wrong procedures can irritate skin. In pigment prone skin, irritation can create post inflammatory hyperpigmentation, which can overlap with melasma and make it look “stubborn”.
Types of melasma
Dermatologists often describe melasma by where the pigment sits in the skin. A Wood’s lamp exam or dermoscopy may help guide decisions.
| Type | Where pigment sits | Typical look | What it means for treatment choices |
| Epidermal | More superficial | Brown patches with clearer borders | Often responds better to topical plans |
| Dermal | Deeper | Grey or grey brown tone | Harder to treat, slower results, needs patience |
| Mixed | Both depths | Combination of brown and grey tones | Often needs a combined plan and longer timeline |
Comparison lesson: Many people waste money because they assume all pigmentation responds the same way. Melasma type affects what is worth paying for and what has higher risk of rebound.
Solutions explained: what actually works for melasma
1) Sun protection (the highest return step)
If melasma keeps coming back after treatment, the most common reason is that triggers are still active. Sun protection is not optional.
A dermatologist guided plan usually includes:
- Broad spectrum sunscreen (often SPF 30 to 50) daily
- Reapplication when outdoors
- Hats, shade, and avoiding peak sun
- Extra protection near windows (UVA can pass through glass)
Trend insight: Tinted sunscreens are getting more attention for melasma because iron oxides can help protect against visible light in addition to UV. This can be especially relevant for people who notice melasma worsening even with “regular” sunscreen.
2) Melasma treatment cream (topicals that target pigment safely)
A melasma treatment cream usually works by slowing pigment production, improving skin turnover, and calming inflammation.
Dermatologists commonly use ingredients such as:
- Hydroquinone (often in controlled cycles)
- Azelaic acid
- Kojic acid
- Tranexamic acid (topical)
- Retinoids (only if your skin tolerates them)
- Vitamin C and other antioxidants
Strategic advice: Do not start many strong actives at the same time. If your skin barrier gets irritated, pigmentation can get worse, not better. A slower plan often produces a better long term result.
3) Prescription or oral options (medical decision)
Some patients may be candidates for prescription strategies, including oral tranexamic acid, depending on their medical history and contraindications. This must be decided by a qualified dermatologist.
4) Chemical peels (carefully chosen)
Superficial peels can help in selected cases, especially when combined with strict sunscreen and a gentle routine. But stronger is not always better. The wrong peel depth, wrong timing, or poor aftercare can trigger post inflammatory hyperpigmentation.
Lesson learned: Many people chase “fast peeling” results. With pigment, slow and steady often gives better outcomes.
5) Lasers and energy based treatments (use with caution)
Lasers are not automatically the best choice for melasma. Some devices can help selected cases, but heat and inflammation can also trigger rebound pigmentation.
This is why diagnosis and settings matter. Be careful with offers that skip proper evaluation and go straight to packages.
If you are searching locally for the best dermatologist in kollam or a trusted skin doctor in kollam, a good sign is when the clinic:
- Confirms it is melasma and not a different pigment condition
- Explains timeline and recurrence risk in simple words
- Starts with barrier repair and sun protection, not procedures first
- Plans follow ups and adjusts treatment if irritation appears
Data and trend snapshot (actionable, not complicated)
Melasma is a common reason people seek dermatology care for pigmentation concerns. A large global review published in 2023 reported wide prevalence ranges across populations, with higher rates in women and in darker skin types.
Instead of focusing only on “how common”, it helps to translate evidence into decision making. Below is a simple “market style” view of melasma solutions, showing what tends to be a foundation (lower risk, high consistency) vs an add on (higher variability).
| Option | “Role” in a plan | Upside | Risk if used wrongly | Best for |
| Sunscreen and visible light protection | Foundation | Reduces flares and helps other treatments work | Underuse leads to quick relapse | Everyone with melasma |
| Topical pigment control (melasma treatment cream) | Foundation | Gradual, steady improvement | Irritation if too strong or layered | Most mild to moderate melasma |
| Chemical peels (superficial) | Add on | Can speed tone improvement | PIH if too aggressive | Selected patients with good aftercare |
| Device based treatments | Add on | Can help some stubborn cases | Rebound pigment, heat trigger | Very selected cases with close supervision |
Mini chart: what usually drives results over time
This is not a promise, but it reflects a practical pattern seen in clinics: consistency beats intensity.
| Step | When you may notice change | Impact on recurrence risk | Common mistake |
| Daily sunscreen and visible light protection | Immediate (prevents worsening) | High | Using sunscreen only on “sunny” days |
| Consistent topical plan | 6 to 12 weeks | Medium | Switching products too often |
| Procedures (peels, devices) when appropriate | Weeks to months | Low to medium | Doing procedures without maintenance |
Real world investor examples: how people spend wisely on melasma
Think of Melasma Treatment like investing. Results tend to come from consistent, lower risk steps first, then higher risk options only when needed.
Example 1: The “quick fix” spender
A patient spends repeatedly on strong procedures hoping for immediate clearance, but skips daily sunscreen and uses harsh products at home. Results are short lived and pigment returns.
Lesson: Without daily trigger control, procedure spending usually has poor returns.
Example 2: The “long game” planner
Another patient invests first in sunscreen, a simple routine, and dermatologist guided topical therapy. They track flare patterns (sun, heat, hormonal changes). After stability, they add in clinic options only if needed.
Lesson: This approach usually delivers more predictable results and fewer setbacks.
Example 3: The “maintenance investor”
A patient achieves improvement, then switches to a maintenance plan (sunscreen, gentle brightening activities, periodic dermatologist check ins). They accept that melasma can recur, so they plan for prevention.
Lesson: Maintenance is not failure. It is risk management.
A simple routine framework to discuss with TLC Skyn
Your dermatologist will personalize your plan, but this structure is common.
Morning
- Gentle cleanser
- Targeted topical (if prescribed)
- Moisturizer if needed
- Sunscreen (broad spectrum, applied well)
Night
- Gentle cleanser
- Melasma topical plan (as advised)
- Moisturizer and barrier support
If your skin feels irritated, a safe strategy is often to pause strong actives and repair the barrier before restarting.
What to ask a dermatologist before you start
Choosing the right plan often matters more than choosing the most expensive product.
Good consultation questions:
- Is this melasma, post inflammatory hyperpigmentation, sunspots, or a mix?
- What triggers are most likely for my lifestyle and climate?
- Which melasma treatment cream approach is safest for my skin type?
- What results are realistic in 8 to 12 weeks?
- What is my maintenance plan after improvement?
For local searchers, these questions also help you choose the best dermatologist in kollam or the right skin doctor in kollam for melasma care.
FAQ
What is melasma treatment, in simple words?
Melasma treatment is a planned routine to lighten patches and reduce how often they return. It usually includes sunscreen, a melasma treatment cream, and sometimes clinic treatments.
How long does melasma treatment take to show results?
Many people see early improvement in about 8 to 12 weeks with consistent sunscreen and topical care. Deeper or mixed melasma can take longer and often needs maintenance.
Which melasma treatment cream is best?
The best option depends on your skin type, sensitivity, and how deep the pigment is. Dermatologists often choose ingredients like azelaic acid, tranexamic acid, retinoids, kojic acid, or short cycles of hydroquinone.
Can melasma be cured permanently?
Melasma often improves a lot, but it can come back when triggers return (sun, heat, hormones). That is why maintenance is part of smart melasma management.
Are lasers safe for melasma?
Some device based treatments can help selected cases, but melasma can also worsen if heat or irritation triggers pigment. It should be done only after proper evaluation.
When should I see a skin doctor in Kollam for melasma?
If patches are spreading, returning often, or not improving with gentle skincare and daily sunscreen, a dermatologist assessment at TLC Skyn can confirm the diagnosis and build a safer plan.